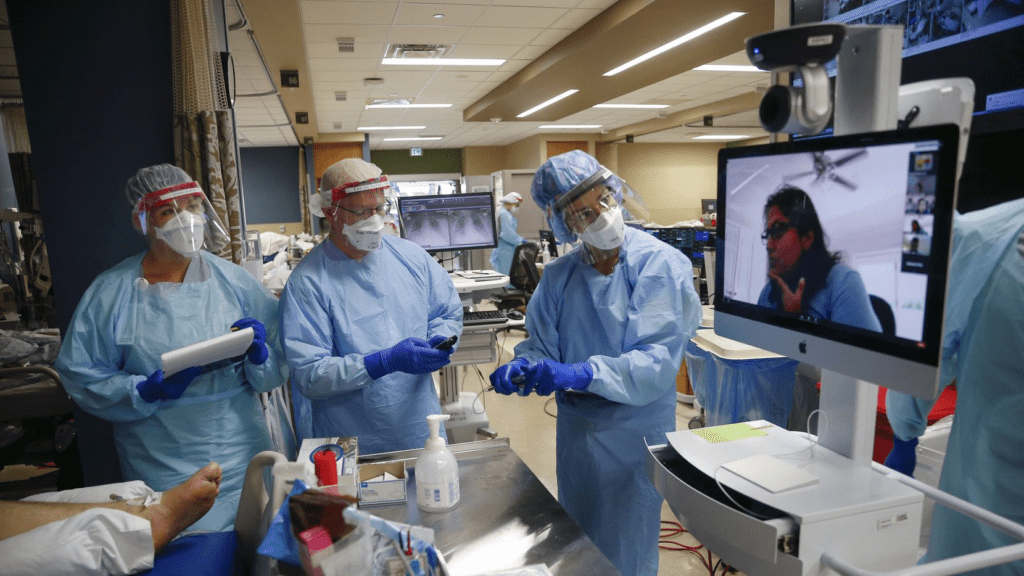
Marsha Maurer, DPN, RN, (Nursing, BIDMC), discusses how the surge of COVID-19 patients impacted hospitals in the Boston region.
Dallas Morning News – July 10, 2020
‘Very, very difficult’: Texas COVID-19 hospitalizations at record high, nearing overwhelming level
Officials are preparing portable buildings and concert venues to house patients as they seek more help to relieve beleaguered doctors and nurses.
AUSTIN — In South Texas, a school district is turning over portable buildings to be used for hospital space. In San Antonio and Austin, concert and convention venues are being prepped as field hospitals. In North Texas, Medical City Healthcare opened more COVID-19 units this week, and Parkland Hospital had to request a disaster assistance team.
Texas is entering a dire new phase of the coronavirus epidemic. Hospitalizations for COVID-19 keep climbing to record levels, and the state health department on Friday said it had no prediction for when that will stop.
As cases surge, hospitals say they have space to add more beds, but lack staff. The state is scrambling to send them more.
Meanwhile, Gov. Greg Abbott is warning the worst is yet to come. The second-term Republican has now canceled elective surgeries in over 100 counties to free up more bed space. On Friday, he hinted another statewide lockdown could be necessary but gave no indication when that might happen.
Over the last two weeks, the number of Texans hospitalized for COVID-19 has climbed every day, from about 5,500 at the end of June to more than 10,000 on Saturday.
“We don’t see a leveling off happening in the immediate future,” Parkland’s chief medical officer, Dr. Joe Chang, said in a statement Friday. “At this point, we simply don’t know when that will occur.”
Record highs
Texas hit record highs last week in all major measures used to judge the severity of the outbreak.
The 58,670 positive cases reported last week account for almost one-quarter of the state’s total cases to date. And of the state’s 3,112 deaths, almost 300 were reported in the last three days.
Dallas County is in the middle of a similar surge, logging more than 7,800 cases over the last week, a quarter of the county’s cases since the epidemic began.
Although the state says there are more than 11,000 beds available across Texas, in some regions, such as Houston, hospitals are already overwhelmed. Others expect their crush to come soon and are preparing.
The Rio Grande Valley has been hit especially hard. Nearly 1,300 people are currently hospitalized with COVID-19 in the region, taking up almost half the area’s hospital beds that are still needed for typical medical emergencies such as heart attacks, car accidents and strokes.
On Friday, Texas’ U.S. senators and three members of congress from the region called on the federal government to set up an emergency field hospital in the Rio Grande Valley. Nine of the area’s 12 hospitals were unable to accept patients on Friday.
“Unfortunately, with recent surges in COVID-19 cases over the past several weeks, our health systems have been pushed to their limits,” said the letter to Health and Human Services Secretary Alex Azar. “COVID-19 cases in South Texas are at their highest peak since the pandemic began, with no indication that case counts will level out soon.”
Before Memorial Day, DHR Health hospital in Hidalgo County had only a few patients, and none in the serious infectious disease unit, said Dr. Carlos J. Cardenas, a hospital executive. Now, there are “upwards of 170 patients in the hospital with COVID-19 and we are holding people in the emergency department.”
The McAllen school district voted this week to lease a dozen portable buildings to hospitals there that need extra space, according to the McAllen Monitor.
On Friday afternoon in a neighboring county, Starr County Memorial Hospital was struggling to transfer three patients on ventilators to bigger hospitals, because they were too sick for the facility to handle. Three more were expected to be intubated within hours and would also need to be moved.
The hospital had tried sending the patients to other facilities in Texas, Oklahoma, Louisiana and other states, but none could take them, said its board president, Dr. Jose Vasquez.
“The situation here is very, very difficult,” he said. “We have seen such a tremendous surge in the number of cases and in the severity of illness here in the Valley.”
Sending staff
In North Texas, the growth of cases is accelerating — now doubling every 18 days — an unsustainable pace, experts say.
“We are concerned that there’s a misconception in the community that this rate of growth can continue without any consequences, and of course there are,” said Medical City Healthcare’s chief medical officer, Dr. Miguel Benet.
Area hospitals have been adding capacity but could have to implement surge plans in two or three weeks, said Steve Love, head of the Dallas-Fort Worth Hospital Council.
“Do we currently have capacity? Yes,” he said. “But we are looking to the future. And we know we are probably going to get a bump for Fourth of July activities.”
The ability to expand depends on staff. More than three months into the epidemic, nurses and doctors are facing burn out.
In coronavirus wards, where patients can be on ventilators for weeks, staff substitute for family. Visitors aren’t allowed, except in some cases where a loved one is approaching death. Day after day, nurses give not only medical care but also emotional support.
“It’s draining at every level,” said Marsha Maurer, chief nursing officer at Beth Israel Deaconess Medical Center, who served as the hospital’s incident commander during the wave of cases that hit Boston this spring.
Hospitals across Texas are turning to staffing companies, retirees and the government for help.
Medical City is pulling staff from areas of the country that aren’t experiencing severe COVID-19 outbreaks, Benet said, and asking nurses to pick up extra shifts.
The Department of State Health Services has deployed over 2,300 doctors, nurses and other medical staff to hospitals statewide, spokesman Chris Van Deusen said. The state has also supplied hundreds of ventilators and other needed medical equipment.
Forty staff were sent to Nueces County, where Corpus Christi is located. The hospital there that’s taking the bulk of coronavirus patients began with 24 COVID-19 beds. Now, there are 178 and plans to add 26 more, County Judge Barbara Canales said.
She worries it will not be enough.
“I have a state school that has 100 positives and a jail that has more than 100 positives,” she said.
The federal government is also helping add staff, said Nim Kidd, who leads the Texas Division of Emergency Management. The U.S. Department of Health and Human Services approved seven disaster medical assistance teams for Dallas, Houston, Austin, San Antonio, the Rio Grande Valley and El Paso, he said.
On Friday night, Abbott announced more resources for the Houston area, including an Urban Area Medical Task Force from the U.S. Department of Defense.
On Monday, Parkland Memorial Hospital expects to get additional staff from government sources.
“This is a good start,” said spokesman Michael Malaise. “We appreciate the help and we hope to get more staff the following week.”
The Department of Defense also sent an 85-member team to San Antonio, Kidd said.
Thirty percent of admissions into hospitals there are now for the coronavirus, said Mayor Ron Nirenberg.
The numbers are rising so quickly that as soon as hospital beds are added, they’re filled with new COVID-19 patients, he said. The city has converted Freeman Coliseum, an event center that usually hosts concerts and trade shows, into a 250-bed hospital, should it be needed.
Are masks enough?
As hospitalizations and cases continue to grow, it remains to be seen whether Abbott’s recent moves — including closing bars and mandating masks —- can reverse the trend.
On Friday, Abbott said in television interviews that his mask order should be enough to contain the spread, if people follow it. But if the mask requirement is not successful, he said, there will have to be another lockdown.
A decision to shut down the state isn’t imminent, he said.
Asked this week how high COVID-19 hospitalizations in Texas could go before he considers further restrictions to slow the virus’s spread, Abbott did not respond.
The state’s crisis was predictable. One of Abbott’s top medical advisers, former U.S. Food and Drug Administration commissioner Mark McClellan, said Texas opened too quickly, before it had pushed the virus into a decline.
The effects of Abbott’s recent restrictions won’t be apparent for at least another week, he said.
“Looking across the country, there are developed ways to address spread,” he said. “Especially when cases are going at an unsustainable rate.”
Further restrictions on business capacities and restaurants are among several options, McClellan said.
The latest Dallas County forecast from disease specialists at UT Southwestern Medical Center predicts that even with the mask mandate, the number of COVID-19 patients who need hospital care will still climb steeply, at least into August. Staying at home as much as people did in mid-May, the forecast says, is necessary to drive hospitalization rates back down.

