In the fight toward herd COVID-19 immunity, Dan Barouch, MD, PhD (Center for Virology and Vaccine Research, BIDMC) spoke to the importance of vaccine-induced T cell responses, particularly for resistant variants that might partially evade neutralizing antibodies.
Science Magazine – February 16, 2021
How soon will COVID-19 vaccines return life to normal?

SAN DIEGO—Twenty days into the new year, cars were entering a parking lot bumper-to-bumper in the shadow of Petco Park, home of the San Diego Padres baseball team. Arms waving, attendants directed the cars into three lines, which split into four more, and yelled as though the first pitch had already been thrown. “I’m going to load you up, I’m sending you 10, you can stack them!” one attendant hollered to another.
But the Padres don’t play in January.
Instead, Petco Park was home field for this city’s drive-thru COVID-19 vaccinations. For 9 days straight, health workers there had been injecting about 5000 people between 7 a.m. and 7 p.m. Run by infectious disease clinician Shira Abeles of UC San Diego Health—dubbed the “vaccine czar” by the 300 people she manages at the Petco operation—it is the city’s largest vaccination site, focusing on health care workers and anyone 75 or older. Cars moved through stations where workers checked people in, injected them, and then watched them for at least 15 minutes to make sure they didn’t have immediate side effects.
The traffic flow was slow but steady—and no one honked. Above their masks, the visitors’ eyes were smiling. If vaccine hesitancy has an opposite, this was it.
By the end of January, nearly 100 million people around the world had received COVID-19 vaccines, and more than 1 million were getting shots each day in the United States and China. The effort was lagging in Europe, and staggering global inequities remain. The World Health Organization noted on 5 February that 75% of vaccinations have occurred in 10 countries. About 130 countries had yet to inject anyone with a COVID-19 vaccine. Still, the vaccines, shown in clinical trials to have efficacies of up to 95% against symptomatic disease, have finally given the world the prospect of an escape from COVID-19’s long siege. “There is so much hope,” Abeles says.
Now, as vaccination campaigns gain speed, a raft of pressing questions have arisen: Does being immunized mean you won’t spread the virus? When will the campaigns begin to curb the pandemic and allow daily life to return to normal? And what do the new variants of SARS-CoV-2, able to spread faster or evade immune responses, mean for the promise of vaccines? “The reality here is this virus is evolving,” says Lawrence Corey, a virologist at the University of Washington, Seattle, who co-leads the U.S. government–supported network that tests COVID-19 vaccines.
Still, answers are emerging.
How soon will there be an impact?
One month into the U.S. vaccination campaign, Abeles thinks she has seen its effect already. Beginning in mid-December 2020 some 11,000 UC San Diego Health employees began to receive the Pfizer-BioNTech or the Moderna vaccine, both of which contain messenger RNA (mRNA) that directs the body’s cells to make the surface protein from SARS-CoV-2, spike, to trigger an immune response. Despite reports of health care workers hesitant to get the vaccines, 96% of Abeles’s colleagues accepted the shots. Each week, those employees are tested for SARS-CoV-2, which exploded in San Diego county starting in December, even if they are feeling healthy.
At the peak, UC San Diego Health was detecting 20 to 30 infections each day in employees, many asymptomatic. By the third week in January, the number had fallen to just a handful. Abeles emphasizes that the evidence is far from conclusive, but says “we are extremely hopeful” that the link between the drop and the mass vaccination is real.
More compelling, if still preliminary, evidence comes from Israel, home to the world’s most aggressive and best studied immunization campaign so far. A country of 9 million people, Israel has universal health care provided mainly through four HMOs with excellent electronic medical records. The Israeli government negotiated with Pfizer to rapidly roll out its mRNA shots in exchange for sharing data about their impact with the company. Between 19 December and 4 February, 39% of Israelis had received at least one dose of the vaccine. Per capita, that is far higher coverage than in any country other than the similarly small United Arab Emirates (36%).
Nationally, COVID-19 cases and hospitalizations appear to be dropping faster among people 60 or older, the first to receive the vaccines, than among the 40- to 60-year-old segment. And in a 1 February press release, the Maccabi Research and Innovation Center—an arm of one of the four HMOs—noted it had tracked 132,015 of its members over age 60 who had received a vaccine dose in the first 9 days of the immunization campaign. Diagnosed SARS-CoV-2 infections in that group peaked about 10 days after immunizations began. By day 28, when most people had received their second, booster dose, diagnoses had fallen by two-thirds, and COVID-19–related hospitalization had dropped from a daily high of seven people to one. In the general population, the team notes, reported cases dropped much more slowly.
Initial impact
Israel’s aggressive COVID-19 vaccine rollout targeted the elderly first, and an analysis of 132,015 people 60 and older who received their initial dose in late December 2020 suggests the shots already started reducing the toll of the pandemic in that country 1 month later.
(Graphic) N. Desai/Science; (Data) Maccabi Research and Innovation CenterThat finding constitutes “persuasive evidence of real-world benefit of vaccination, especially since prior behavioral restrictions in Israel did not seem to selectively protect those over 60,” says Roby Bhattacharyya, an infectious disease specialist at Massachusetts General Hospital.
In the United States, people living in long-term care facilities, most of them elderly, and facilities’ staff were put at the front of the line for vaccines. Those residents account for about 40% of the country’s COVID-19 deaths, so the impact of vaccinations on their hospitalization and mortality will probably be seen “within a month or two, certainly,” says Ira Longini, a biostatistician at the University of Florida (UF).
The effect may have already become visible. COVID-19 cases have been dropping nationwide since December, including at nursing homes. Interventions other than vaccines explain some of the fall. But a county-level comparison of facilities that got their first shots from 18 to 27 December and those that didn’t showed the drop in daily cases was more than twice as large in the earlier vaccinated facilities (a 48% decline versus 21%).
Blunting COVID-19 cases nationwide is a long game, however, especially in a country such as the United States, where the vaccine rollout has not been as fast or uniform as in Israel. “We have a big country. We have a lot of transmission,” Longini says. “I don’t think we’ll see a big impact on numbers of cases” from vaccines until the summer.
Will vaccination stop you from spreading the virus?
If vaccines created what’s known as sterilizing immunity all the time, no vaccinated person would transmit the virus. Vaccinated grandparents could safely play with their unimmunized grandchildren. Countries could welcome visitors who had proof of vaccination with little fear of introducing new viral variants or reigniting outbreaks.
That level of assurance is a tall order. Few vaccines, for any infectious diseases, create sterilizing immunity—even the most effective ones. The inactivated poliovirus vaccine developed by Jonas Salk did little to block infection or transmission of the virus, yet it powerfully prevented paralytic polio. By 1961, 6 years after it was licensed, only 54% of the U.S. population had received the vaccine, yet paralytic polio cases had dropped by more than 90%.
For practical reasons, the recent COVID-19 vaccine efficacy trials evaluated mainly the frequency of symptomatic disease, typically detected after participants feel sick and get a virus test. It’s tougher to identify all SARS-CoV-2 infections, which remain invisible if they don’t cause symptoms. Yet models suggest asymptomatic cases account for about half of transmission, so tracking them among vaccine recipients is key. “There are easy ways to look at transmission and hard ways,” says Ruth Karron, who runs the Johns Hopkins University Center for Immunization Research.
One approach, says John Mascola, who heads the Vaccine Research Center at the National Institute of Allergy and Infectious Diseases (NIAID), is to ask: “If you’re vaccinated, could you have the virus in your nose and shed it?” That’s how researchers studying the AstraZeneca–University of Oxford vaccine recently tried to get at transmission. In a U.K. efficacy trial of that vaccine, participants did weekly nasal swabs at home. Results showed vaccination reduced asymptomatic infections by 49.3%. The data suggest, but do not prove, that the vaccine stymies viral spread; misleading news coverage claimed the vaccine had cut transmission by two-thirds. Moderna has also reported a similar decline in asymptomatic infections after just one dose of its mRNA vaccine in a subset of its large efficacy trial, which found overall that the vaccine had 94% efficacy against mild disease.
Several COVID-19 vaccine studies have opted for a simpler, if less precise, look at the issue. They took repeated blood samples from people in both the placebo and vaccinated groups at different time points. The trials tested for antibodies against the viral N protein, which are triggered by infection but not by most vaccines. If the placebo group has more positive N antibody tests than the vaccinated group, that would suggest the vaccine had cut asymptomatic infections—and therefore transmission. No group has yet reported results from those “serosurveys.”
Early data from Israel indicate vaccinated people who nevertheless became infected with SARS-CoV-2 have reduced levels of virus, which may make them less contagious. A research team from the Maccabi group and the Israel Institute of Technology measured viral loads in nasal samples taken from more than 1000 people who became infected between 12 to 28 days after their first dose, the period in which immunity begins to build. The amount of virus found was significantly less than in a similar group of unvaccinated, infected Israelis, the group reported on 8 February in a preprint on bioRxiv.

AMIR LEVY/GETTY IMAGES
Myron Cohen, an infectious disease clinician at the University of North Carolina, Chapel Hill, and colleagues at the COVID-19 Prevention Network have a proposal at NIAID to study the question in college students. One group would receive the vaccine immediately and a control population would get it weeks later. Both groups of students would swab their noses daily to assess whether there are differences in the rate of asymptomatic SARS-CoV-2 infections and levels of the virus. Withholding vaccine would be ethically dodgy if doses were plentiful, but most college students are still not eligible for vaccination, and they are less likely to develop serious COVID-19 than older adults. Cohen is confident the trial will receive the necessary ethical approvals.
Knowing whether vaccines stop transmission may not matter to government officials. “In the next 6 months, we’re probably going to have a menu of vaccines and each is going to have characteristics related to the cold chain, number of doses required, reactogenicity, and efficacy,” Karron notes. “We’re going to make policy decisions about use based on all of those characteristics. I don’t think that some superimprecise measure of transmission is going to be one of the things that goes into our calculus.”
But Cohen contends that the difficult studies to evaluate whether immunized people spread the virus are worth doing. “Unless we answer this question, we are a masked society. We need to address this to become maskless.”
When will we get back to normal?
That depends on the definition of normal. To many people now, it means herd immunity, in which a high percentage of a population has either been vaccinated or naturally infected, leaving too few susceptible hosts for a virus to continue to spread. “It’s such a clean, beautiful concept, the tipping point idea, that if we can just get there, the virus will go away, and then we can just go about our business as if it’s gone,” Longini says. “It’s kind of a pie-in-the-sky concept that’s very, very attractive.”
The idea of herd immunity, a term imported from livestock veterinarians, has become more beguiling as huge swaths of populations in parts of the world recover from SARS-CoV-2 infections, leaving them with some degree of immunity. In India, for example, serosurveys have found antibodies to the virus in about half of people in the city of Delhi and the entire state of Karnataka. And though no one is claiming this meets the herd immunity threshold, new cases have recently dropped precipitously.
Still unclear is what percentage of a population needs to be vaccinated or recovered from COVID-19 before herd immunity kicks in. Early predictions were between 60% and 70% and then rose as high as 90%—but that’s all based on modeling or even guesswork. Anthony Fauci, who heads NIAID, has been taken to task for changing his own estimates. Recently on CNN, Fauci acknowledged that: “I think we all have to be honest and humble. Nobody really knows for sure.”
Recent developments have been sobering. The COVID-19 vaccines rolling out are highly effective against hospitalization and death, but their success against mild and moderate symptoms plummets when faced with viral variants that can evade vaccine-triggered antibodies. And herd immunity, even if it emerged, could easily fade as immunity waned or new variants arose.
Yet there is growing recognition that even if widespread vaccination can’t halt the spread of the virus, it promises a major step back toward normal. Preventing severe disease and death in the elderly and people with comorbidities such as obesity and hypertension—the most vulnerable—is still a resounding victory over the virus, many epidemiologists say.

Large swaths of the population might still become infected and develop minor disease or asymptomatic infections. That prospect worries some scientists and clinicians, who note that even mild cases can lead to the “long COVID” phenomenon of lingering symptoms. Hospitals, though, will not become overwhelmed with emergency cases and deaths will become increasingly rare.
To Corey, those metrics are the most relevant. “When will the ICU use and all of this decant so that we’re at the point where, yes, we can sort of tolerate this?” he asks.
“We’re not going to shut down this virus and end transmission,” agrees Nicole Lurie, an adviser to the Coalition for Epidemic Preparedness Innovations. “We have to make a decision as a society about how much of this we can and want to live with.” Society lives with influenza, after all, which remains endemic despite a vaccine. But Lurie stresses that flu is not an appealing model. It kills up to 60,000 people per year in the United States alone—a toll she would not want to accept from COVID-19.
Still, immunologist Brigitte Autran, a member of France’s Scientific Committee on COVID-19 Vaccines, says herd immunity isn’t needed to bring back normalcy. “The first goal is to have individual protection, and by summing the individual protections, to have a protection of the society that will allow countries to come back to almost real, true lives.”
How much of a threat do viral mutants pose to immunity?
That concern quickly moved from the theoretical to the real world when multicountry studies recently revealed several vaccines were least effective against symptomatic COVID-19 in South Africa. That’s where 95% of infections now stem from a viral variant that in test tube studies could dodge antibodies against the viral spike protein. Novavax’s protein-based vaccine went from 89.3% protection in the United Kingdom, where the variant is rare, to 49.4% in South Africa. And South Africa even halted its planned rollout of the AstraZeneca-Oxford vaccine, which consists of a harmless viral “vector” carrying the gene for the spike protein, after a small trial there indicated the vaccine had 22% efficacy.
Still, the vaccine-triggered immune responses may retain plenty of muscle, enough to prevent serious symptoms. A third vaccine, from Johnson & Johnson, also fell short against mild disease in South Africa, but it prevented almost all severe disease—with no hospitalizations or deaths. (The AstraZeneca-Oxford and Novavax studies were too small to address impact on severe disease.)
One explanation could be that the level of key spike antibodies, those capable of “neutralizing” SARS-CoV-2’s infectivity, jumped so high after vaccination that there was a cushion: Even though several labs reported that the variant in South Africa reduced the impact of the vaccine-induced antibodies by up to ninefold, if those immune fighters rise to high enough levels they may still pack enough punch to thwart serious disease.
Other arms of the immune system less affected by the mutations in the variant likely contribute to protection. Pfizer and BioNTech have shown their mRNA vaccine triggers a steep increase in key T cells. One set, which carries the CD8 receptor, targets and destroys cells that SARS-CoV-2 manages to infect. Underscoring the importance of those cells, Pfizer and BioNTech found that even though neutralizing antibody levels triggered by their vaccine were minimal in the 21 days between the first and second doses, it still gave 52.4% protection against disease during that period. “Vaccine-induced T cell responses are important for COVID-19 vaccines, particularly for resistant variants that might partially evade neutralizing antibodies,” suggests Dan Barouch of Harvard Medical School, whose lab has documented the importance of CD8+ cells for protecting monkeys from coronavirus reinfection.
Mixing and matching COVID-19 vaccines may also boost both antibody and T cell responses to higher levels, creating bigger cushions. Studies of various combinations have begun.
Will the variants change the course of the pandemic?
That’s the realm of modelers like Longini. Often, they restrict their analyses to tight geographical areas, which makes it easier to amass high-quality data and to account for variables that can alter outcomes. So Longini and Thomas Hladish, also at UF, created a model for their home state that extrapolates from actual case numbers for COVID-19 and assumes a rapid rollout, starting with people older than 65, of vaccines that are 60% effective at preventing infection. Assuming the virus doesn’t change, they found that a vaccination campaign reaching half the population would slash symptomatic disease and death by 30% by August.
Surprisingly, their Florida model shows COVID-19 cases would steadily decline even without vaccination. That’s because the state’s reproductive number for SARS-CoV-2—how many other people each COVID-19 case infects—has dropped below 1. “It’s mostly masking, social distancing, and the slow buildup of natural immunity in the population,” Longini says. Indeed, as in many U.S. states, Florida’s cases began to drop steeply in January.
But that decline could quickly reverse if a mutant strain takes off that’s 50% more infectious, such as the B.1.1.7 variant strain that exploded first in the United Kingdom and has come to the United States, including Florida. “We will have a much bigger epidemic that starts happening now,” Longini says. But with more viral spread, the impact of vaccination would be bigger, averting twice as many symptomatic cases and deaths.
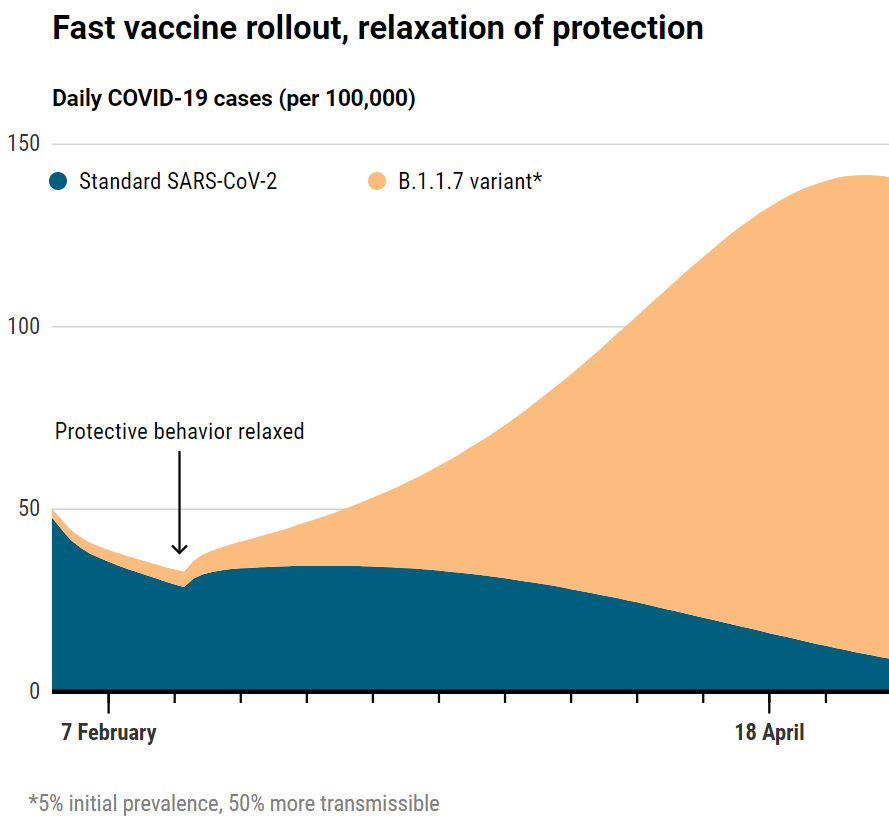
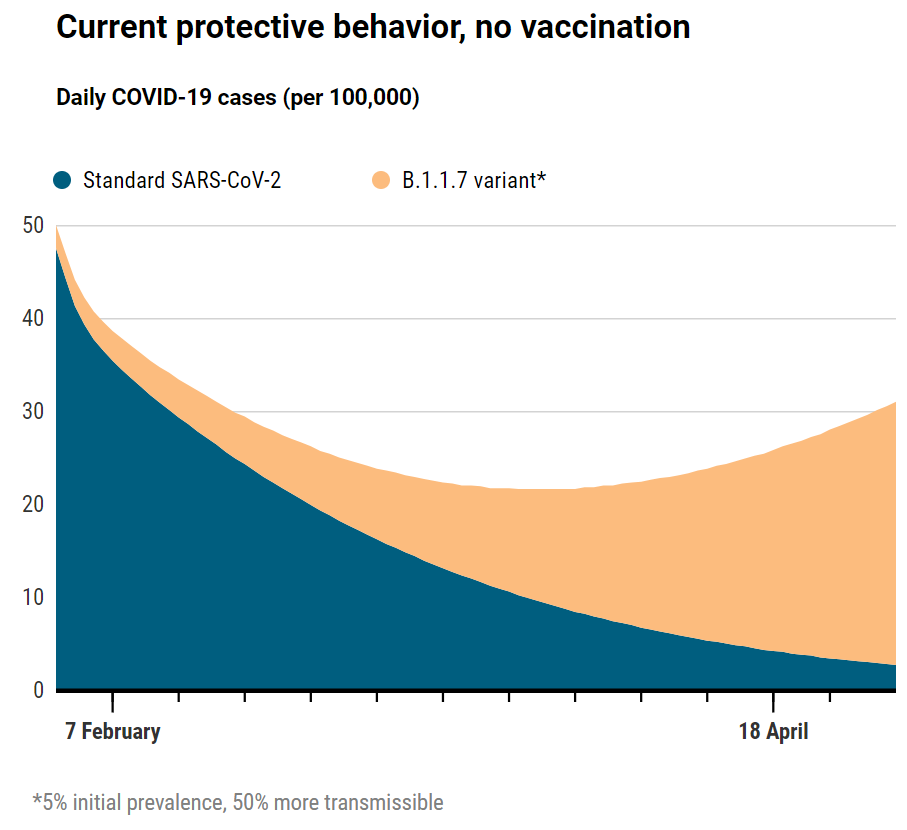
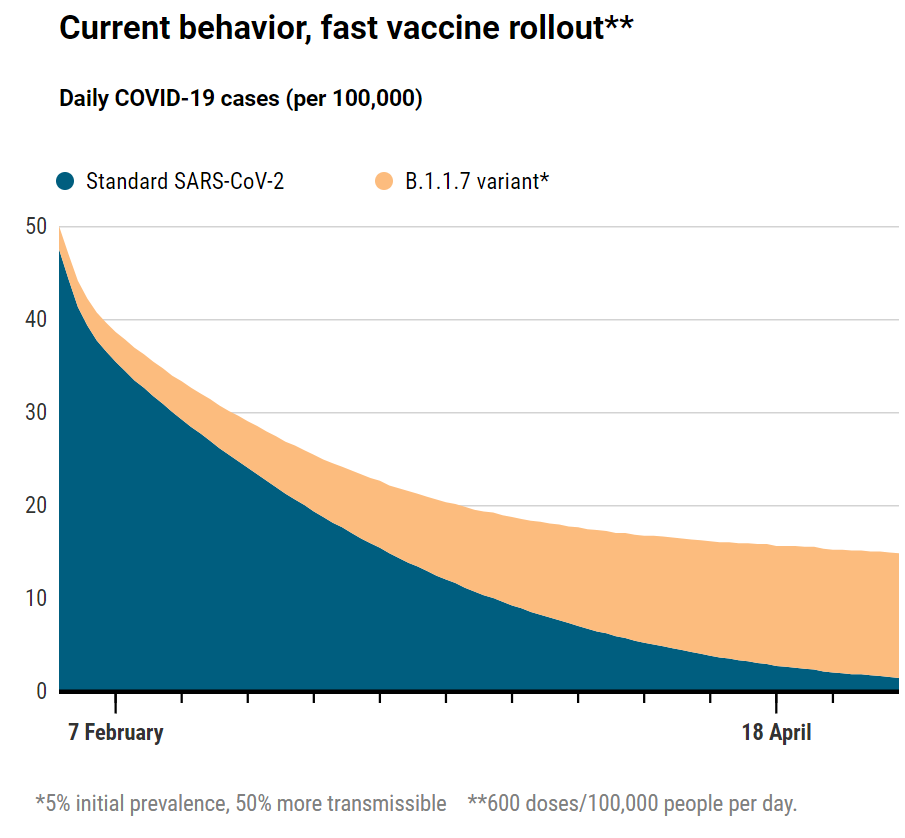
Vaccines versus variant
Models suggest the impact of COVID-19 vaccinations in San Diego will be blunted by the fast-spreading B.1.1.7 variant, which already accounts for 5% of SARS-CoV-2 infections there. If other prevention efforts are relaxed, a surge of cases will swamp the gains from vaccination.
Modeler Natasha Martin and her team at the University of California, San Diego, have looked at the interplay of variants and vaccines in an even smaller area: their home county. Sequencing of COVID-19 cases in San Diego county has shown the highly transmissible B.1.1.7 variant has a 5% prevalence so far—10 times higher than recently estimated for the nation. Martin’s model shows that if the variant takes over, as many researchers expect, aggressive vaccination campaigns over the next 3 months will still cut case numbers in half. But if the county drops its guard and people become lax about prevention efforts, COVID-19 cases will triple even with rapid vaccination. “We are at a critical moment in the epidemic, where our progress in terms of declining cases could quickly be reversed as the B.1.1.7 strain expands,” Martin says. “We have the tools we need to fight the spread of this virus: masking, social distancing, vaccination. Now is the time to vaccinate as many people as fast as we can, and double down on masking and distancing.”
How quickly can we tailor vaccines to the new variants?
Vaccine developers proved in 2020 that they can move from concept to candidate vaccine, ready to test in people, in as little as 2 months. Changing the genetic code used in an mRNA or vector-based vaccine, or making a new inactivated-virus preparation, should be at least as fast. (A genetically engineered protein, such as the Novavax vaccine, takes longer.)
But by far the biggest time sink and expense for getting COVID-19 vaccines into use were the large-scale efficacy trials, which took about 4 months. Would those need to be repeated for each updated vaccine? No, says Peter Marks, who heads the vaccine division at the U.S. Food and Drug Administration. All the agency would likely require, he says, is a “modest size” study in humans showing the immune responses elicited by the new vaccine resemble those triggered by the original and are likely to be protective.
Flu vaccines, after all, are updated yearly to keep up with the ever-morphing influenza virus and are quickly approved. Makers can pop out components from the old vaccine and replace them with new ones. Regulators require minimal evidence about the revised product—often just animal studies showing it performs as well as last year’s model.
But with COVID-19 vaccines, no one knows which immune responses correlate with protection. Many vaccine experts assume neutralizing antibodies to the spike protein are the most important driver of protection. To prove that, however, researchers need to compare immune responses between vaccinated people infected by viruses that “broke through” their protection and vaccinated people who did not become infected. A more in-depth “sieve” analysis of breakthrough cases refines the correlates of protection by looking at the genetics of the variants that break through. Those studies are underway, but the Moderna and Pfizer-BioNTech vaccines, the first approved, worked so well that it was difficult to figure out the protective immune responses. “There weren’t that many vaccinated, infected people,” explains Mascola, who is helping coordinate the analyses.
Still, Marks says he anticipates that by the time makers of vaccines formulate new preparations to combat variants and test them in small human studies, the key immune responses will have become clear. “We may well have the correlate confirmed by March when it is really needed,” he says. That could open the way for rapid approval and rollout of boosters designed to keep up with the evolving virus—and ensure that any hard-won progress against the pandemic isn’t undone.