Alexa Kimball, MD, MPH (President & CEO, Harvard Medical Faculty Physicians at BIDMC) shared her experience administering the COVID-19 vaccine to her colleagues.
WBUR – February 2, 2021
‘I Can Dare To Hope’: What It Felt Like To Spend A Day Vaccinating My Hospital Colleagues
It’s a Sunday morning, 6:15 a.m. My alarm goes off, playing Alanis Morisette’s “You Learn.” Throwing on my white jacket and heading to the third floor of the hospital feels different than it did yesterday. I’ve been waiting — we’ve all been waiting — for today for weeks.
I am thrilled, not only because I’m about to get the COVID-19 vaccine but because I’m about to give it. As CEO of a physicians’ group, the feeling of wanting to protect those who have cared for all of us during these tumultuous and scary months, and the happiness at finally being able to, is overwhelming. These are the people who have been directly in harm’s way. They — we all — made a choice when we became physicians to provide health care to others, and we wouldn’t trade that choice. But it is fair to say we never expected this pandemic.
The caregivers who will line up — six feet apart — have sacrificed so much and born witness to so much pain, suffering and loss. Months ago I wanted to wrap them all in safety bubbles of PPE. This morning is my moment to not just say thank you, but to give them the best possible present: the vaccine.
A woman exits the elevator, stands still and declares, “I’m so excited!” to no one in particular.
I start at 7 a.m. and the first people I see are nurses and doctors finishing overnight shifts. They’re tired but relieved. Some have questions. One asks if she can take a selfie so she can show her family that she is finally safe. Of course. A young woman who has just started as an administrative receptionist admits that she’s been a little bit scared — her floor has six COVID patients — but is now relieved. I get the impression that this is her first job. A woman exits the elevator, stands still and declares, “I’m so excited!” to no one in particular. There’s a young woman who’s worried that she might have been exposed to COVID a few days ago and wants to know if getting the vaccine today will be okay. It is.
Giving injections isn’t hard. I’m a dermatologist and I use needles all the time to deliver relief. I know skin so well — its strength and flexibility, its warmth and touch. But to give this vaccine I need to go deeper. There’s the familiar pop that I know to expect as you move through the dermis, the really thick, tough part of skin. And then you get into muscle and the needle slides quickly. Most of the time, there is no bleeding. Turns out, the hardest thing is opening the Band-Aids, which stick to the paper.
The pharmacists are so careful tracking how they draw up this liquid gold, and only give us one or two syringes at a time to make sure that nothing is wasted. The sharps bucket of used syringes is two-thirds full. That’s a good sign. It marks the progress. It’s magic that we have been able to create this salve in less than a year. Science that feels like magic.
I meet Pam, an energetic, enthusiastic infectious disease doctor who has volunteered multiple sessions over the holidays. She cleared her schedule to make sure she could be a part of this public health miracle that is the vaccine. Pam had introduced me to her vaccination protocol: We need to tell our people which vaccine they’re getting — today, it’s Moderna — when to come back, what to expect. I add my own advice: This first dose doesn’t necessarily protect you. Please, please be careful until a few weeks after the second. I refine my methods for maximum efficiency so that I don’t have to touch a pen more than once. I fill out the form that includes the consent, I fill out a sticker that marks the 15-minute mark for their time, so they know how long they need to stay and be observed.
I add my own advice: This first dose doesn’t necessarily protect you.
All the clocks in the cubicle are set 15 minutes ahead so I don’t have to do the math — I can just write down that time. That seems like a good idea. And lastly, I fill out the vaccination card. I don’t have very good handwriting anymore so I fill it out very carefully, as carefully as I can, because I know they’ll probably need this card, and I know it is important.
I get faster, and I could probably do more. There are so many people whom we could help. I make phone calls to bring people in, and bother colleagues on a Sunday morning to ask them to help me. They do so without hesitation. Pam figures out that I am some sort of administrator but helps me keep my cover because today I am mostly just a physician. Fifty of our doctors volunteered over the past few weeks to give vaccinations, and they feel, I expect, just the same way I do.
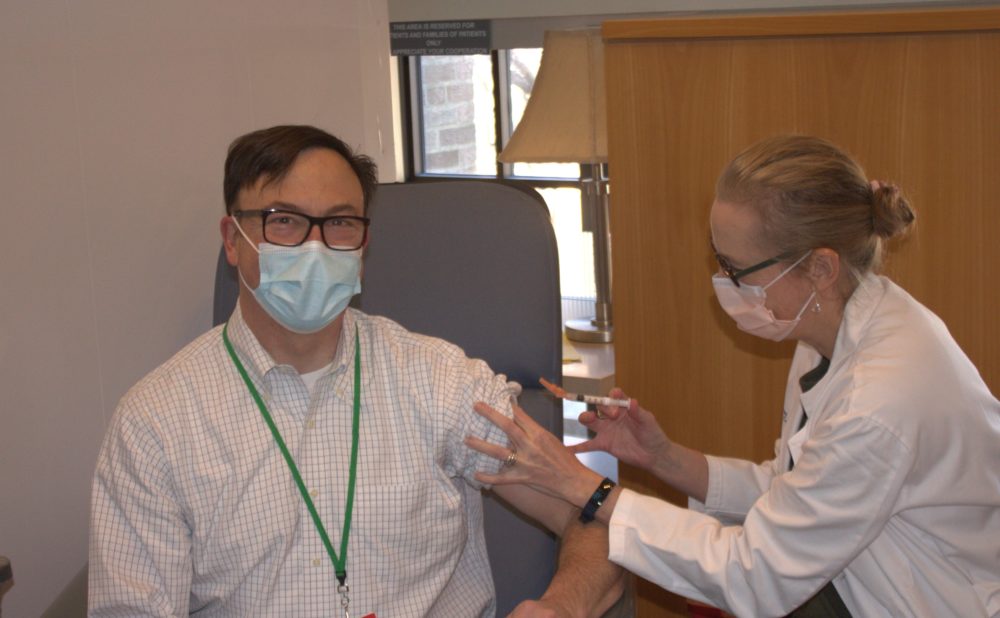
At the end of my shift, my colleague, who has worked tirelessly at my side throughout the pandemic to help our physicians and caregivers and patients, arrives and I give him his vaccination. He wears a dress shirt, marking the enduring professionalism of a physician. We can’t hug but we bump elbows, and that is my final gesture for the day to protect the people who have given so much during this pandemic.
I can dare to hope.

